ENDOCRINE ORGANS (ANATOMICAL MICROSCOPY)
9.8
Thyroid gland
Specimen:
SPECIMEN DETAILS:
Organ: Thyroid gland
Origin: Human
Staining: Hematoxylin Eosin (H&E)
METHOD AND SPECIMEN DESCRIPTION:
Routine histological section stained with H&E, demonstrating the general architecture of the thyroid gland and its two distinct endocrine cell populations.
OBJECTIVE OF THE EXAMINATION:
To study the microscopic structure of the thyroid gland, focusing on its follicular organization, epithelial components, and the presence of parafollicular (C) cells.
Special Features of the Specimen:
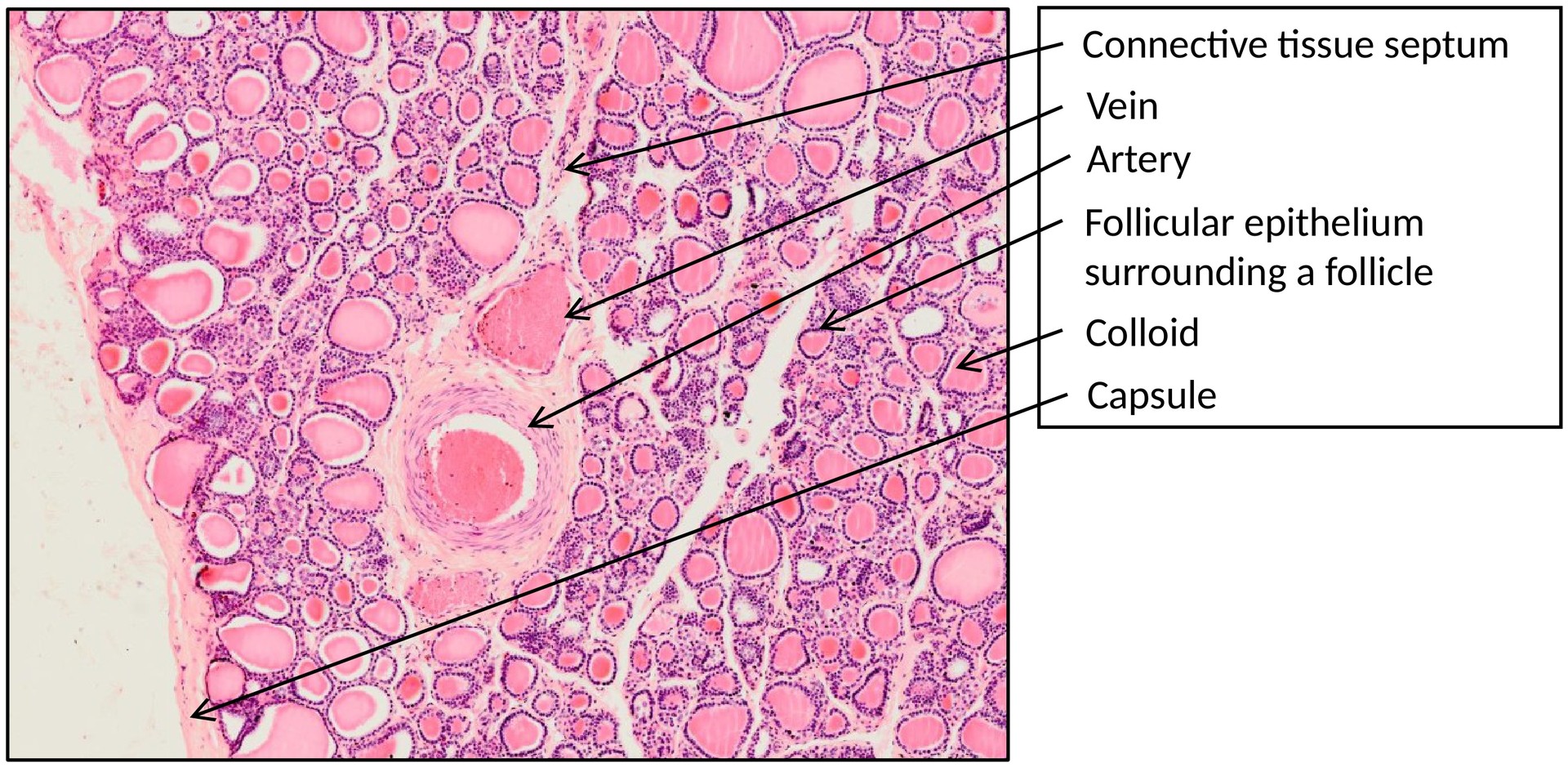
In adults, the thyroid gland consists of two lobes connected by a narrow isthmus. The lobes are located lateral to the thyroid, cricoid, and upper tracheal cartilages and are enclosed by a fibrous capsule that sends connective tissue septa into the gland, dividing it into lobules.
The gland contains two main endocrine cell types:
-
Thyroid follicular (epithelial) cells, derived from endoderm, and
-
Parafollicular (C) cells, derived from the neural crest.
The most striking histological feature is the presence of numerous thyroid follicles — roughly spherical structures filled with colloid, a homogeneous, eosinophilic material surrounded by a single layer of cuboidal to low columnar epithelial cells.
The colloid consists mainly of thyroglobulin, a glycoprotein synthesized by the follicular cells. Thyroperoxidase catalyzes the iodination of thyroglobulin, forming iodinated precursors of thyroid hormones. When stimulated by thyroid-stimulating hormone (TSH), the follicular cells endocytose colloid, cleave iodinated thyroglobulin by proteolysis, and release thyroxine (T4) and triiodothyronine (T3) into the bloodstream.
T4 serves primarily as a prohormone, being converted in peripheral tissues to the more active T3 (triiodothyronine), which increases cellular metabolism and oxygen consumption.
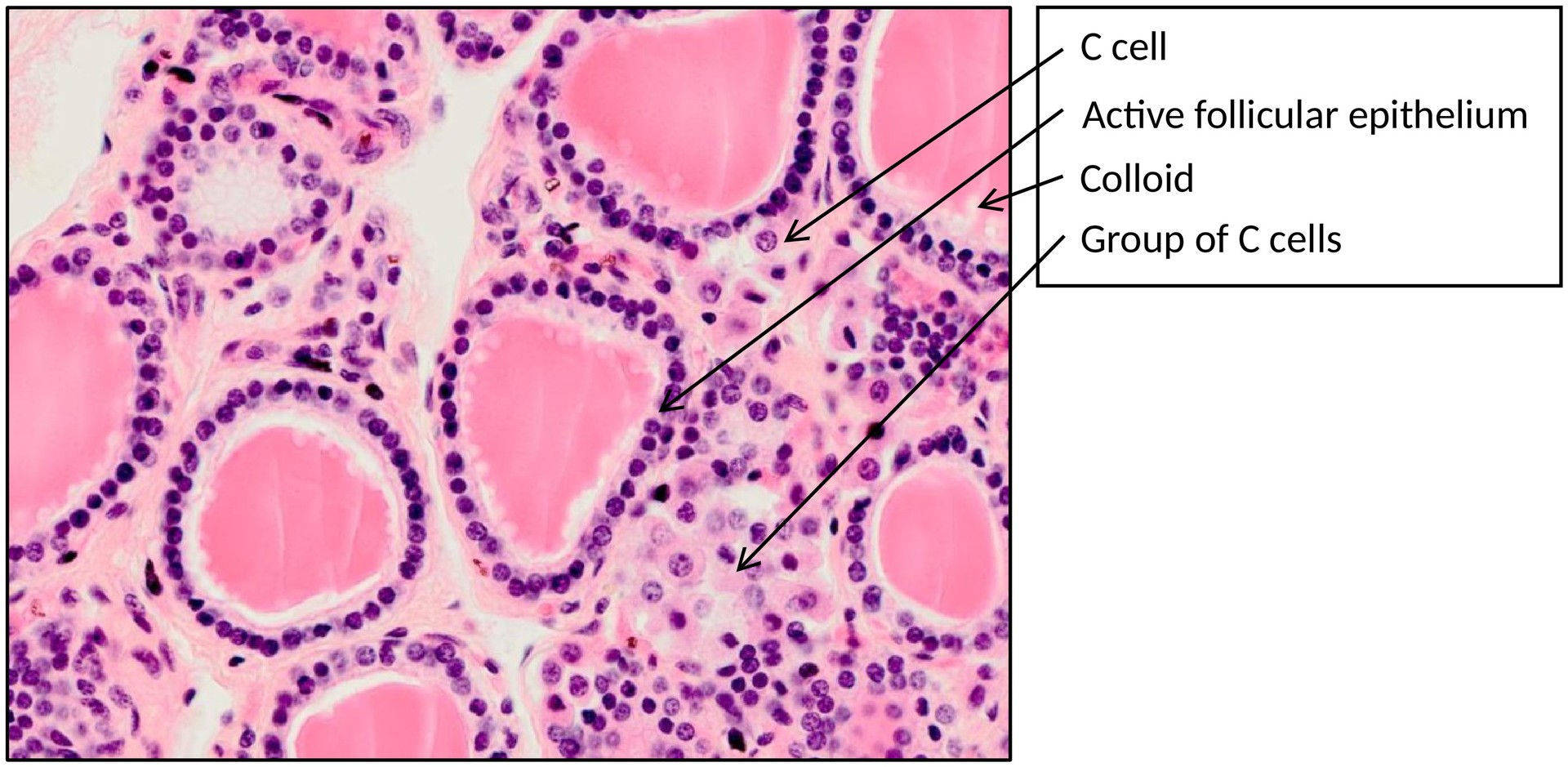
Scattered singly or in small clusters between follicles are the parafollicular (C) cells, which secrete calcitonin. This hormone lowers blood calcium levels by inhibiting osteoclastic bone resorption and stimulating calcium deposition in bone matrix.
TASKS:
• Identify the capsule and the lobular division of the thyroid gland.
• Observe the arrangement and size of the follicles, noting variation in epithelial height and colloid density.
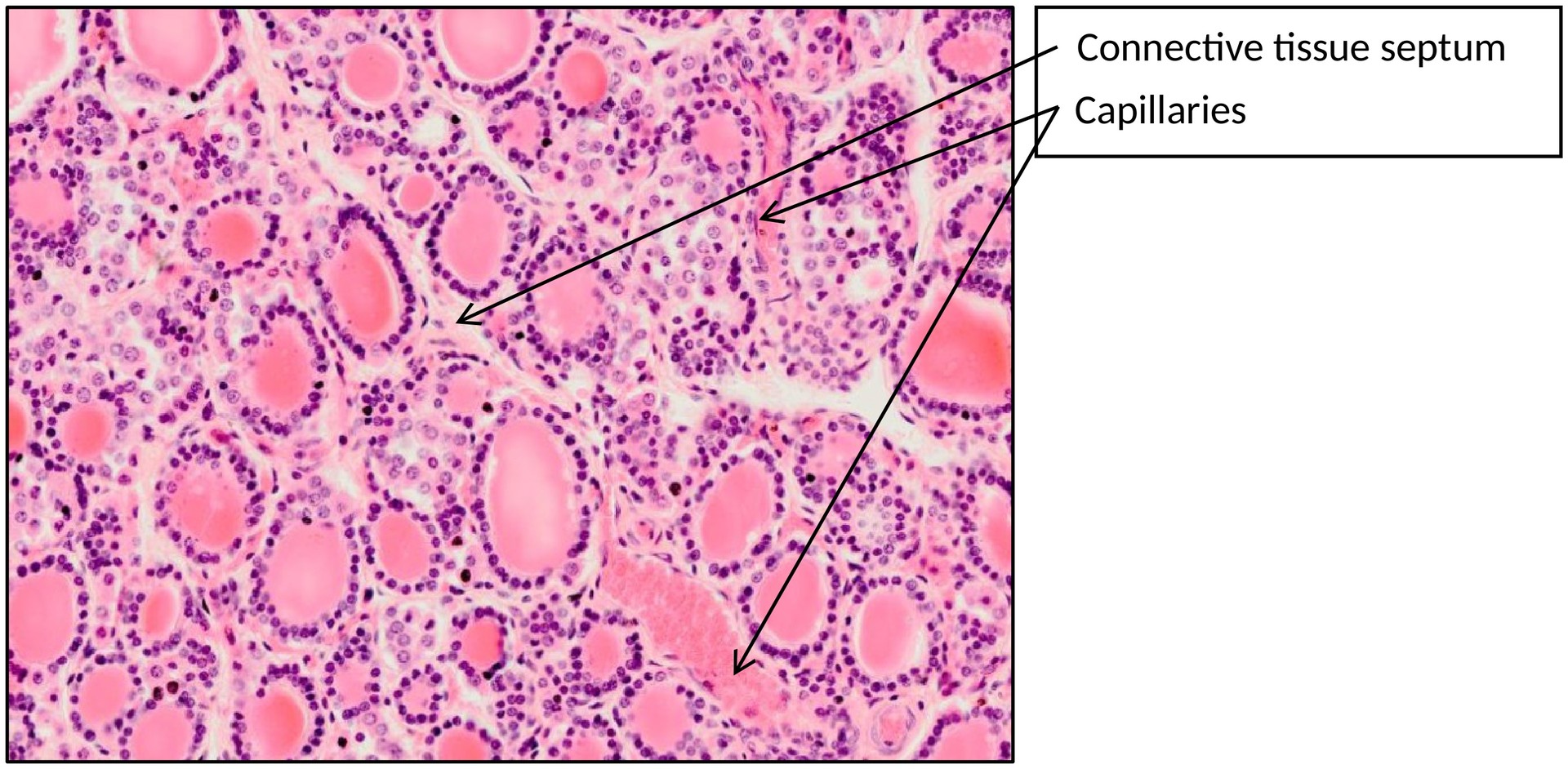
• Locate and describe the follicular epithelium, colloid, capillaries, and connective tissue septa.
• Identify parafollicular (C) cells, typically found in the interfollicular spaces or within the basal part of the follicular epithelium.
License
University of Basel
