GLANDS (GENERAL HISTOLOGY)
3.10
Lacrimal gland
Preparation:
Preparation Details:
Organ: Lacrimal Gland
Origin: Human
Staining: Hematoxylin-Eosin (H&E)
Method and Specimen Description:
Routine histological section stained with a general overview stain (Hematoxylin and Eosin).
Objective of the Examination:
To understand the microscopic structure of the lacrimal gland, a purely serous, tubulo-acinar gland, and to appreciate its functional role in maintaining the hydration and transparency of the cornea.
Special Features of the Specimen:
The lacrimal gland is part of the lacrimal apparatus, which also includes the lacrimal canaliculi, lacrimal sac, and nasolacrimal duct. Its secretions lubricate and protect the ocular surface.
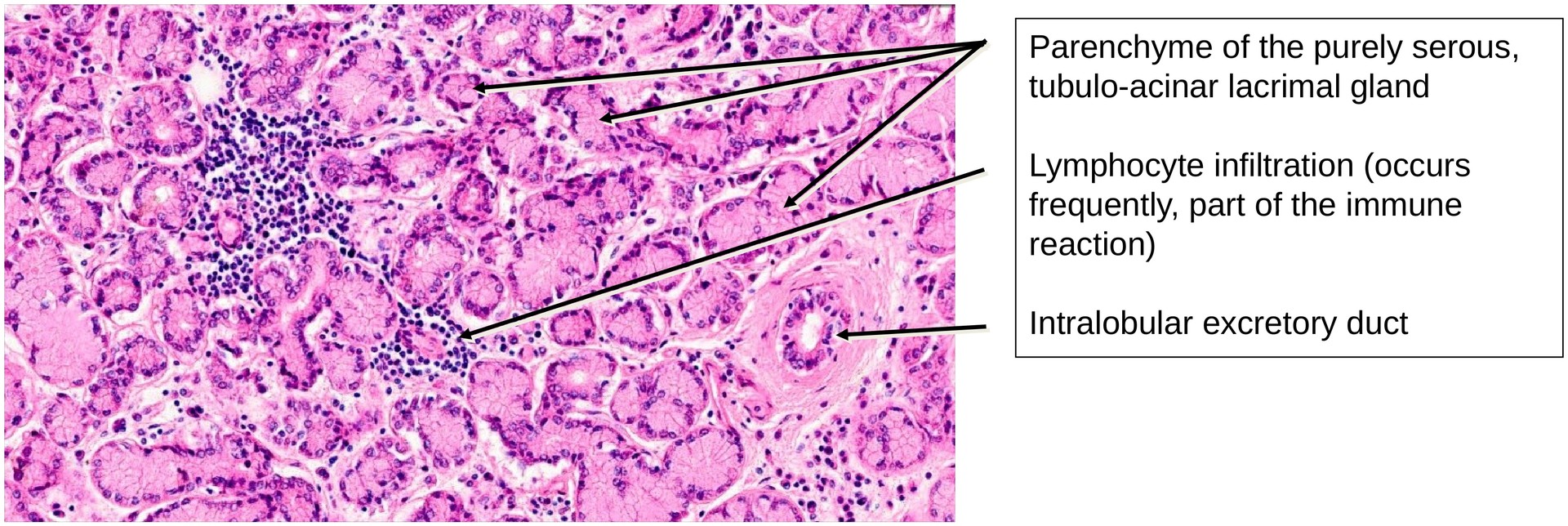
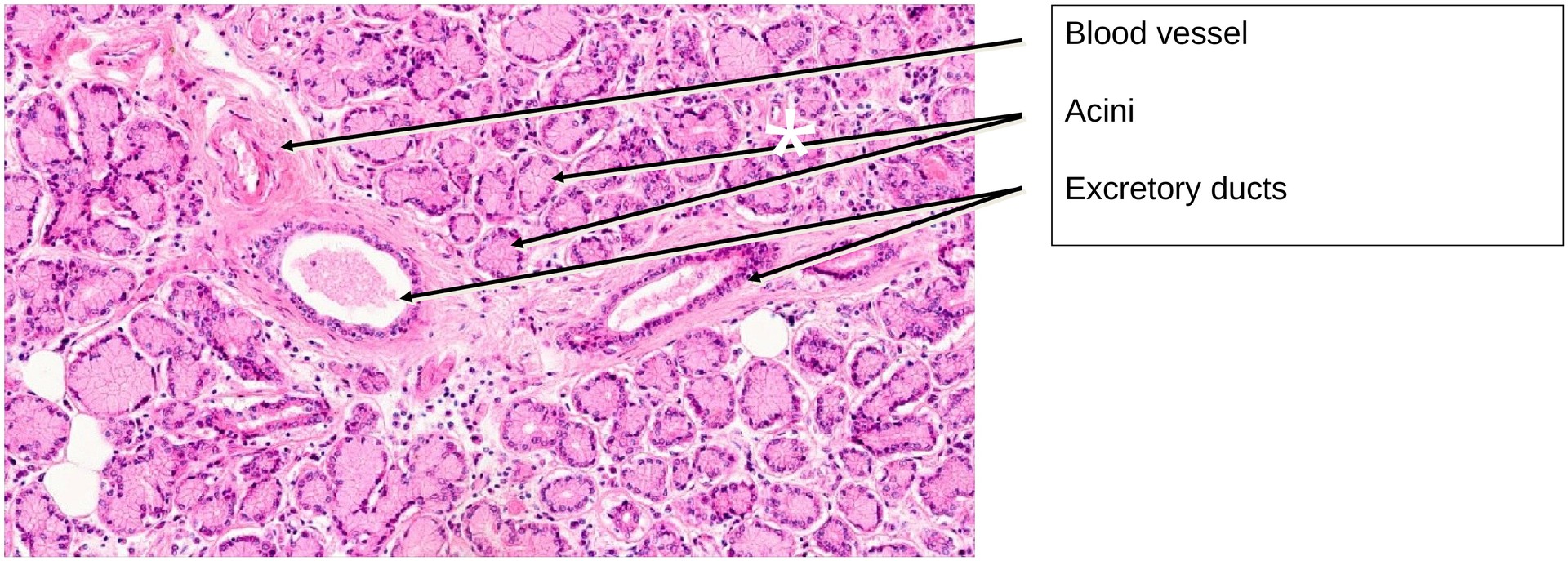
At low magnification, the gland is seen to be divided into lobules by connective tissue septa. Within these septa run vessels, nerves, and excretory ducts. Each lacrimal gland possesses approximately 6–12 excretory ducts, which open into the superior fornix of the conjunctiva, delivering tear fluid onto the ocular surface. This secretion maintains the swelling pressure (hydration) of the cornea—essential for its transparency. If tear production is impaired, corneal desiccation and opacity may result, leading to visual impairment.
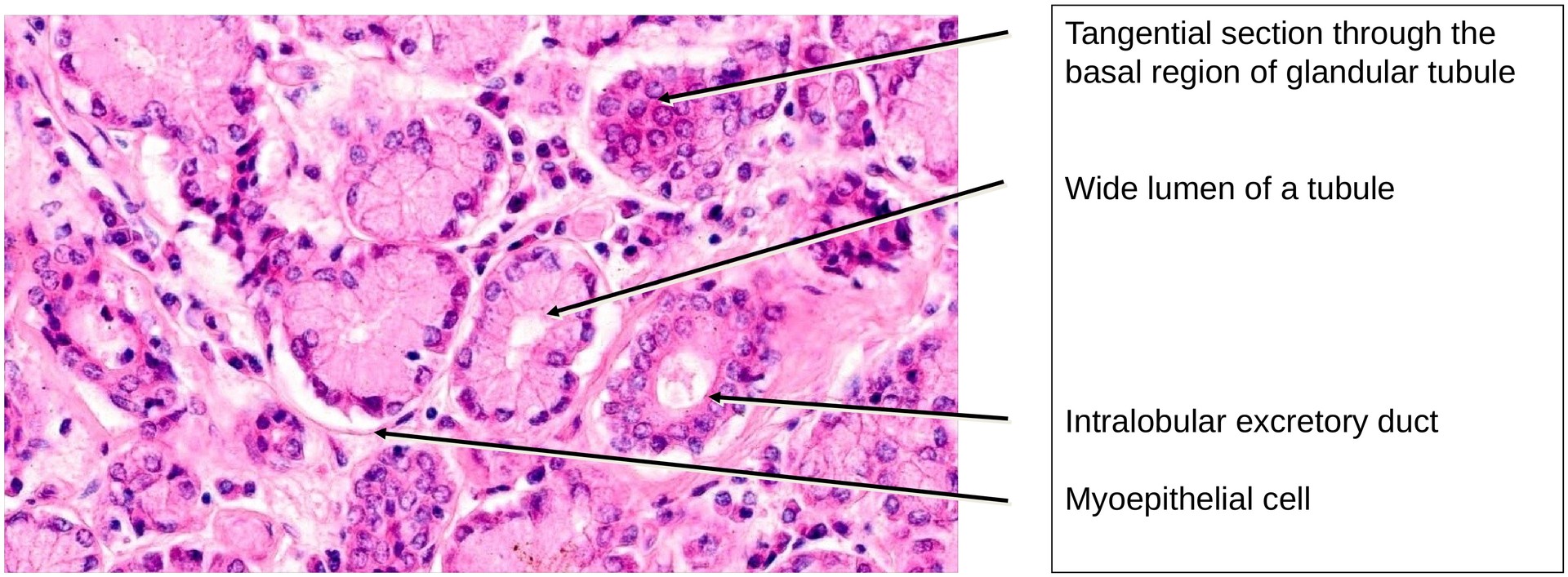
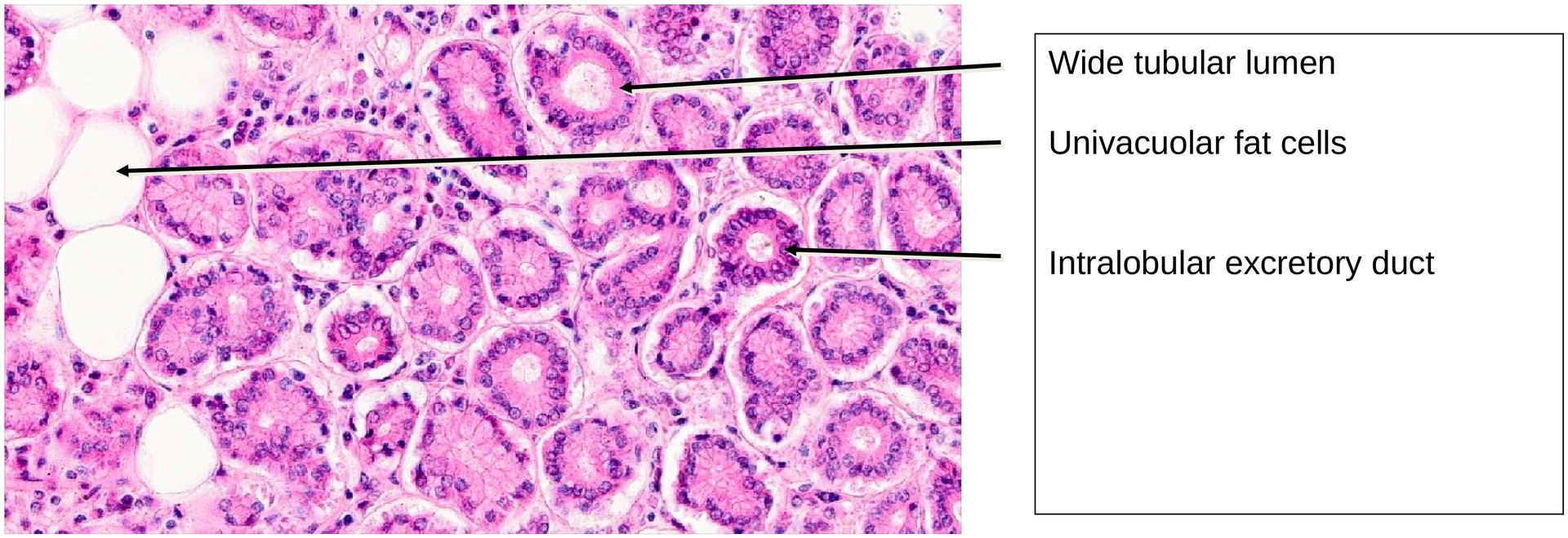
Histologically, the lacrimal gland is a purely serous, branched tubulo-acinar gland. Unlike the parotid gland, it lacks well-defined intercalated and striated ducts. Occasionally, glandular tubules display a slightly wider lumen, giving rise to the description of a tubulo-alveolar structure in some texts.
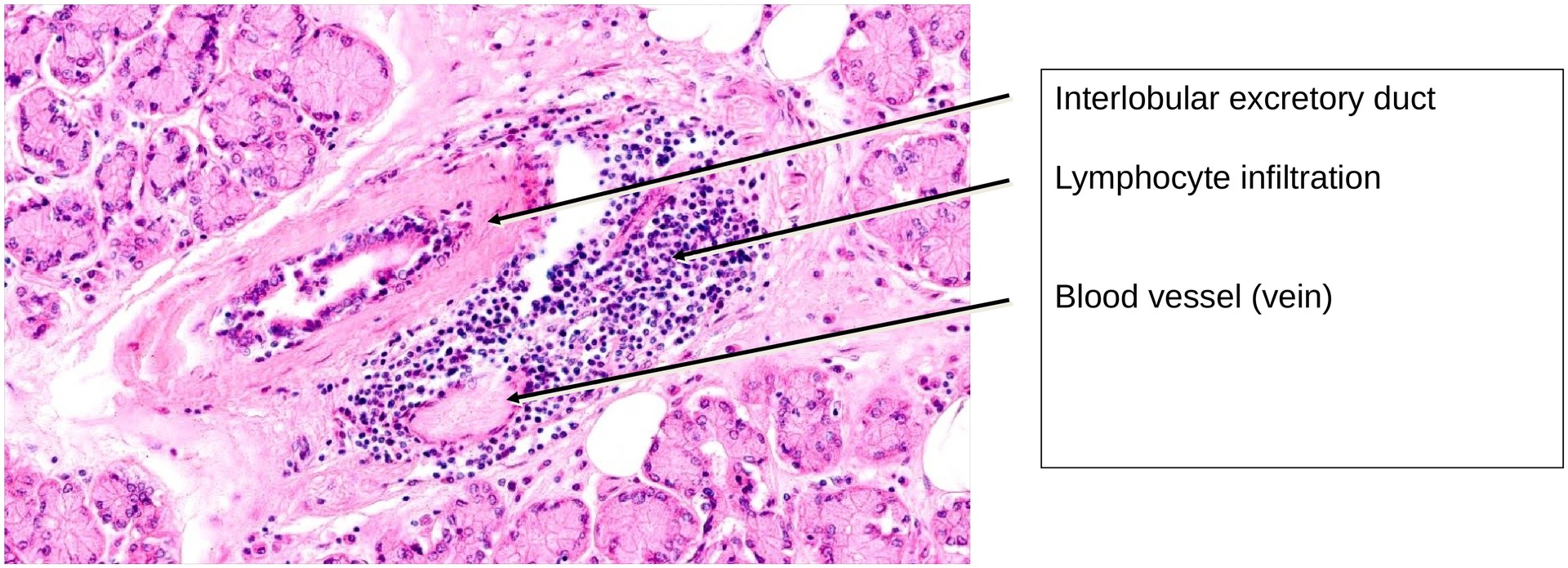
Myoepithelial cells are present around the secretory acini and occasionally along the excretory ducts, aiding in the expulsion of secretion. Univacuolar lipid cells are frequently seen, and their number tends to increase with age. The presence of lymphocyte aggregates or focal lymphocytic infiltrates is typical and reflects the gland’s immune function, contributing to ocular surface defense.
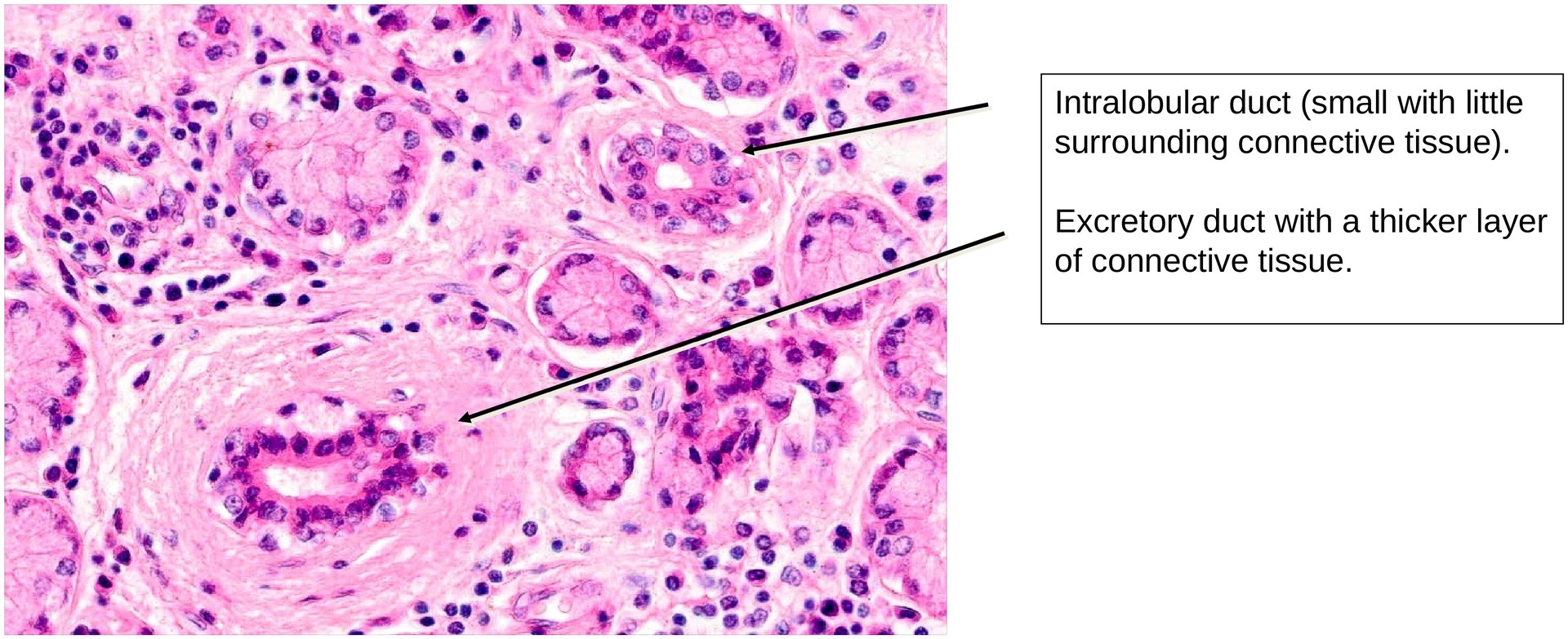
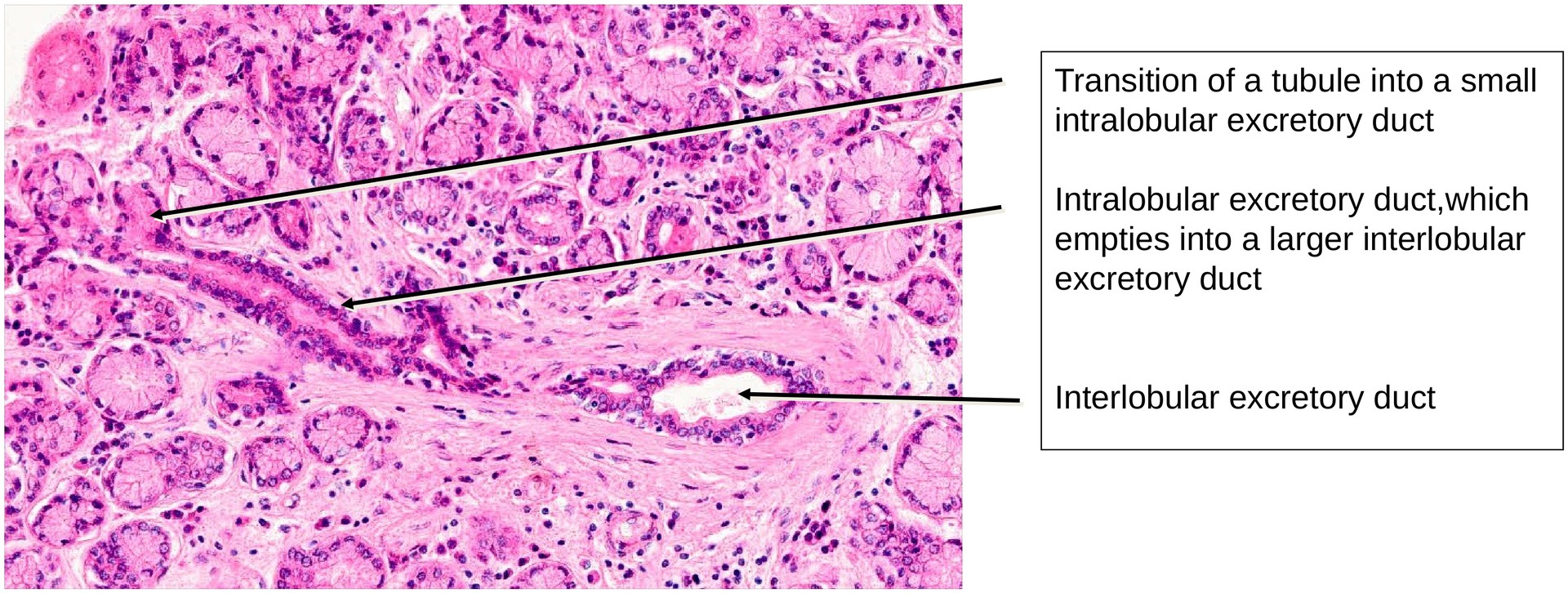
Due to the absence of intercalated and striated ducts, the excretory ducts arise intralobularly. These ducts are distinguishable from the secretory end pieces by their narrower lumina, lack of granular apical cytoplasm, and frequently two or more layers of epithelial cells. The transition between the secretory portions and the ducts is gradual rather than sharply defined.
Nerve fibers, particularly parasympathetic branches, can often be observed in the connective tissue septa, reflecting the gland’s secretomotor innervation.
Tasks:
• Examine the specimen at low magnification to gain an overview of the glandular architecture. Based on its features, determine why this cannot be a section of the parotid gland.
• Identify intralobular excretory ducts and describe their epithelial lining and general characteristics.
• Distinguish between small and large excretory ducts in terms of epithelium and wall thickness.
• Compare secretory acini with small intralobular ducts, noting differences in cell morphology and staining.
• Locate lymphocyte aggregates and explain their functional significance within the gland.
• Search for nerve branches within the connective tissue between lobules and relate them to the autonomic regulation of tear secretion.
Summary Table – Key Features of the Lacrimal Gland
| Feature | Description |
|---|---|
| Type of secretion | Purely serous |
| Structure | Branched tubulo-acinar (often termed tubulo-alveolar) |
| Duct system | No intercalated or striated ducts; only intralobular and interlobular excretory ducts |
| Myoepithelial cells | Present around acini and ducts |
| Lymphocyte infiltration | Common; increases with age |
| Adipocytes | Present, especially in older individuals |
| Distinctive features | Absence of striated ducts, presence of lymphoid tissue and lipid cells, purely serous secretion, parasympathetic innervation |
License
University of Basel
Downloads
