FEMALE REPRODUCTIVE ORGANS (ANATOMICAL MICROSCOPY)
10.1
Vagina
Preparation:
Preparation Details:
Organ: Vagina
Origin: Human
Staining: Hematoxylin - Eosin (H&E)
Method and Specimen Description:
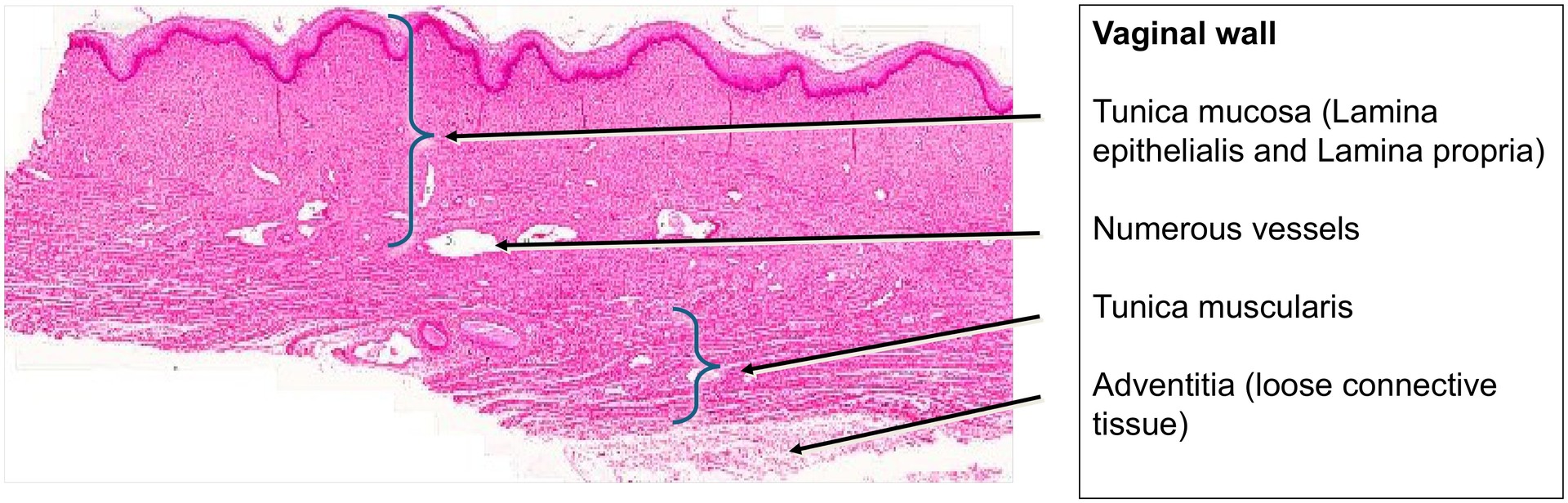
Routine histological section of the vaginal wall stained with a general overview stain (H&E).
Objective of the Examination:
To study the non-keratinized stratified squamous epithelium and the layered organization of the vaginal wall, correlating histological features with function.
Special Features of the Preparation:
The vagina, corresponding to its dual function in sexual intercourse and as a birth canal, exhibits a highly stretchable and elastic wall structure. It lacks glands; therefore, mucosal lubrication arises from two main sources:
-
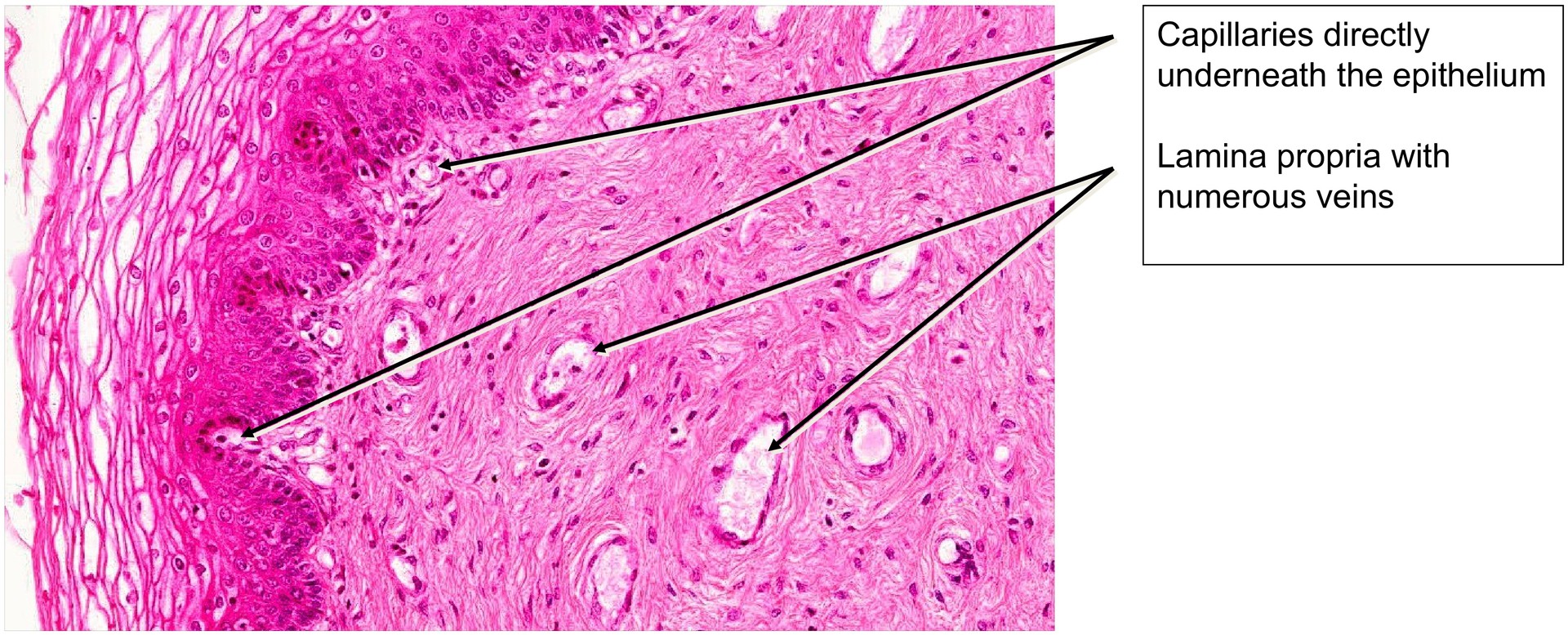
Transudation of plasma from the abundant subepithelial blood vessels.
-
Cervical and uterine secretions descending into the vaginal lumen.
The epithelium appears relatively pale in histological sections due to the loss of intracellular glycogen during tissue processing. In vivo, glycogen accumulation within epithelial cells provides a substrate for Lactobacillus vaginalis, which metabolizes it to lactic acid, maintaining the acidic vaginal pH that inhibits pathogenic bacteria.
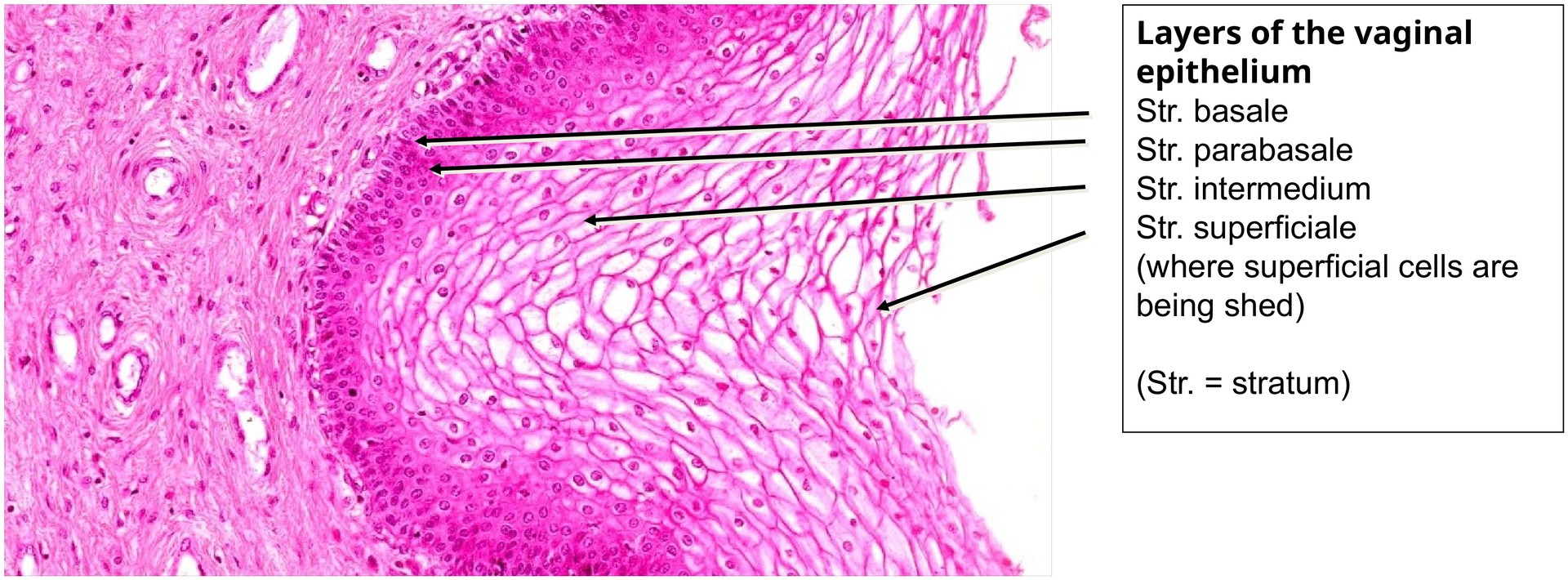
The vaginal epithelium is a non-keratinized stratified squamous epithelium composed of four main strata:
-
Stratum basale – the proliferative basal layer, with densely packed nuclei and high mitotic activity.
-
Stratum parabasale – early differentiating cells above the basal layer.
-
Stratum intermedium – the thickest layer, containing glycogen-rich cells with pale cytoplasm.
-
Stratum superficiale – the most differentiated layer; superficial cells retain nuclei and organelles.
Occasionally, keratohyalin granules may be present in the uppermost layers, but true keratinisation does not occur. Even when these granules are visible, the superficial cells remain nucleated and vital.
The morphology of the vaginal epithelium varies with hormonal changes during the menstrual cycle, particularly under the influence of estrogen and progesterone. These cyclic variations are diagnostically useful, as cytological smears of the vaginal epithelium can be used to assess the stage of the menstrual cycle.
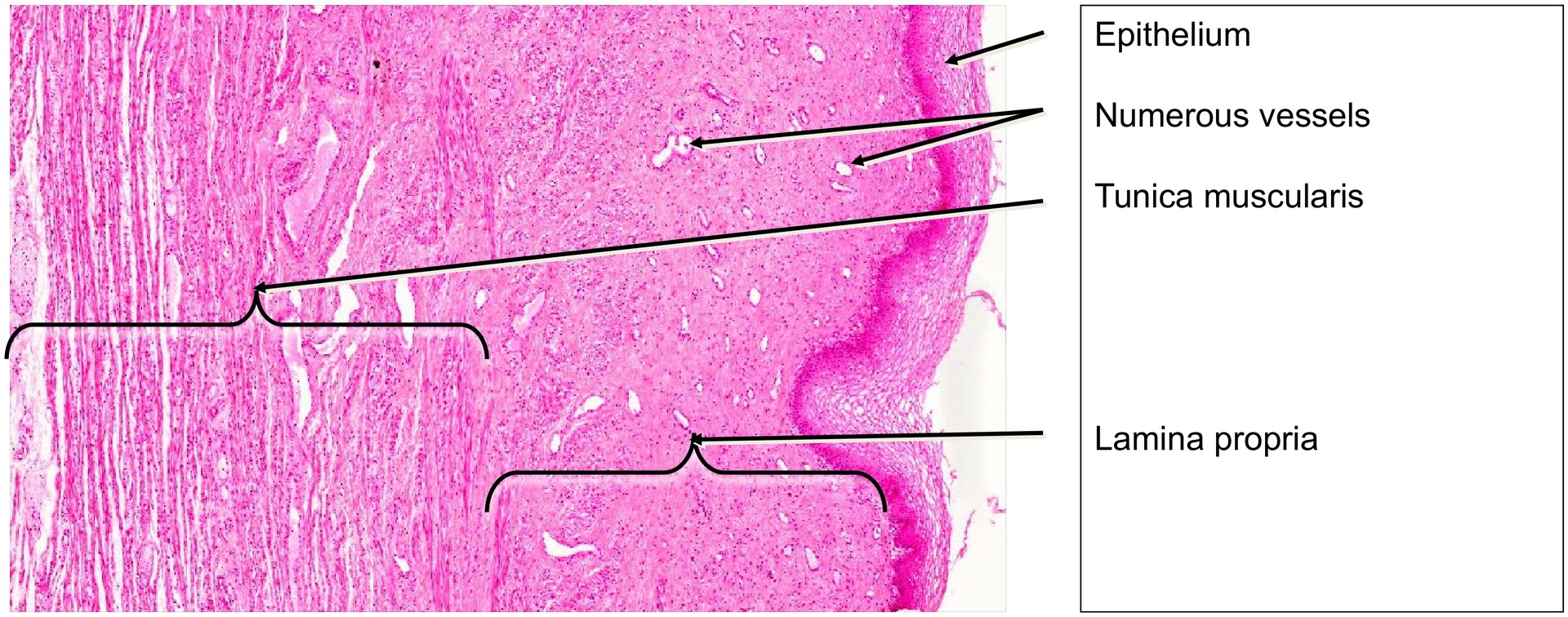
The lamina propria (connective tissue of the mucosa) contains numerous blood vessels, supporting the process of transudation and providing resilience.
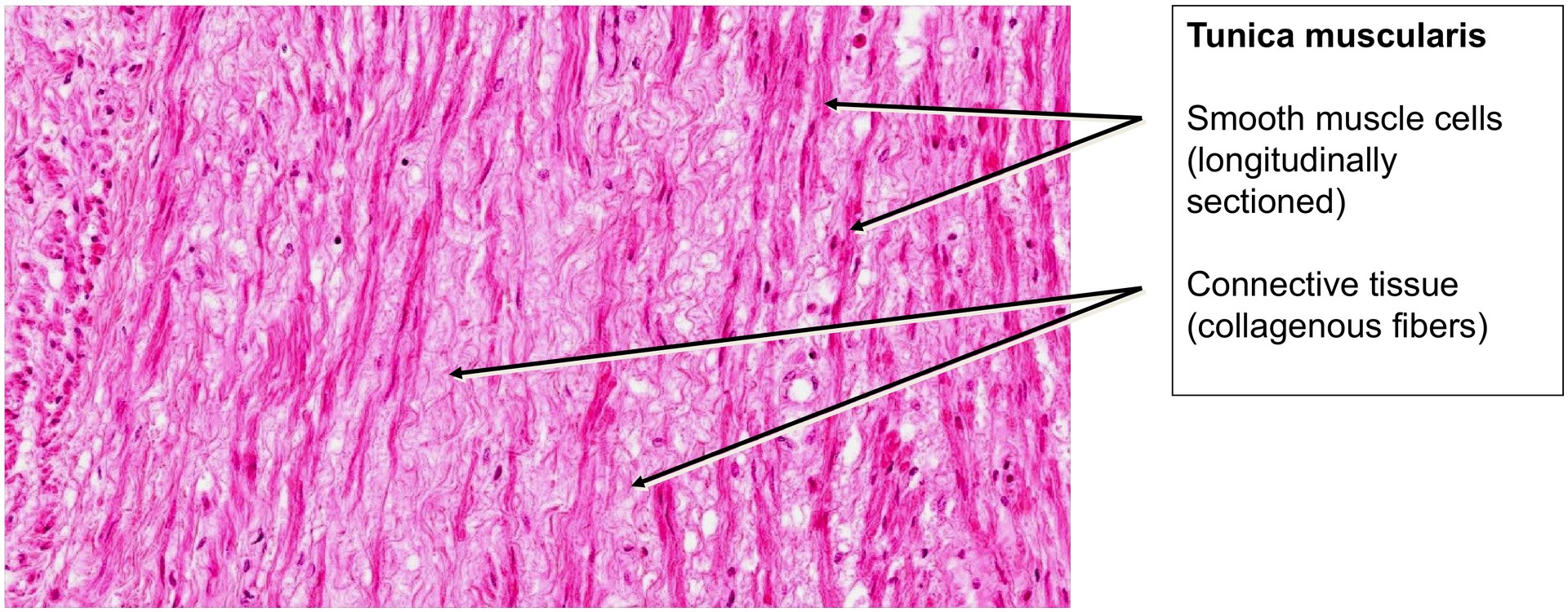
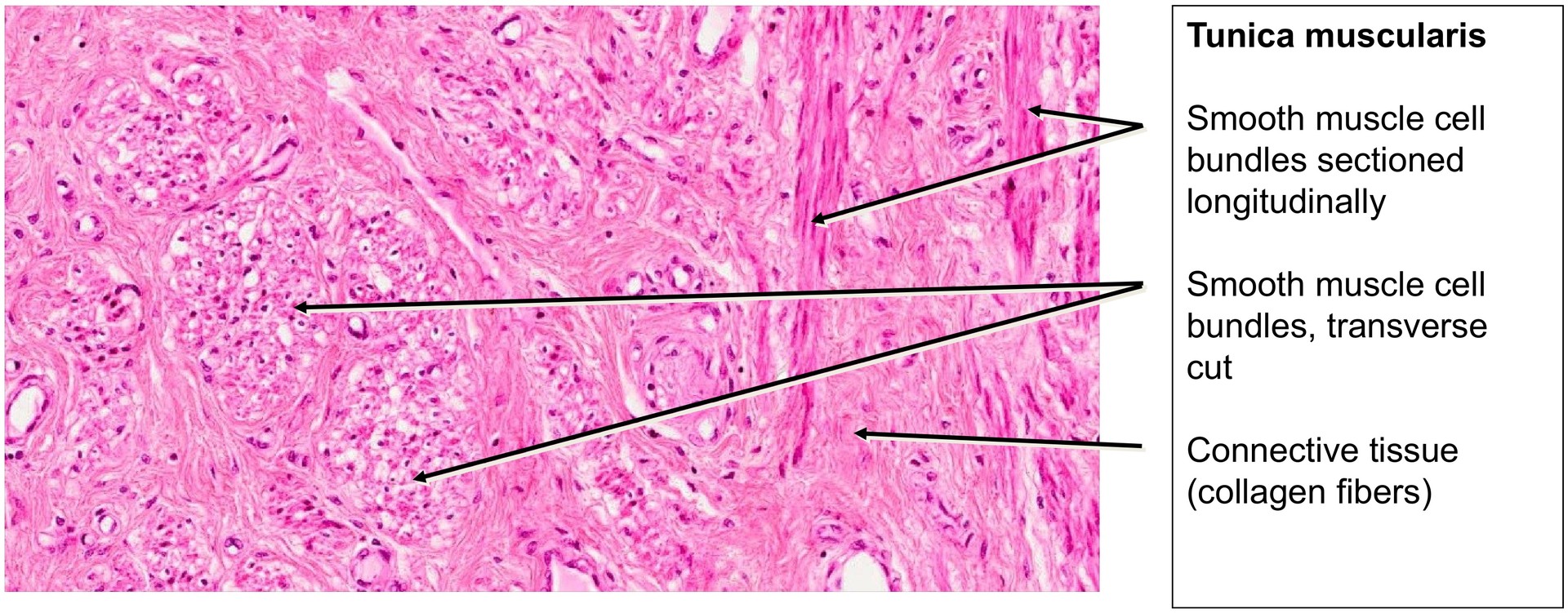
The tunica muscularis is relatively thin and composed of interwoven bundles of smooth muscle cells arranged in varying orientations, with connective tissue interspersed between them.
The outermost adventitia consists of loosely arranged connective tissue, which connects the vagina to surrounding pelvic structures.
Tasks:
-
Examine the section at low magnification to identify:
-
Lamina epithelialis
-
Lamina propria
-
Tunica muscularis
-
Adventitia (visible particularly in the upper right portion of the section).
-
-
Identify the individual epithelial layers:
-
Stratum basale
-
Stratum parabasale
-
Stratum intermedium
-
Stratum superficiale
-
-
Explain why the cytoplasm appears bright (due to glycogen loss during preparation).
-
Examine the lamina propria and note its rich vascularization.
-
Identify smooth muscle bundles within the tunica muscularis.
-
Observe the loose connective tissue structure of the adventitia.
-
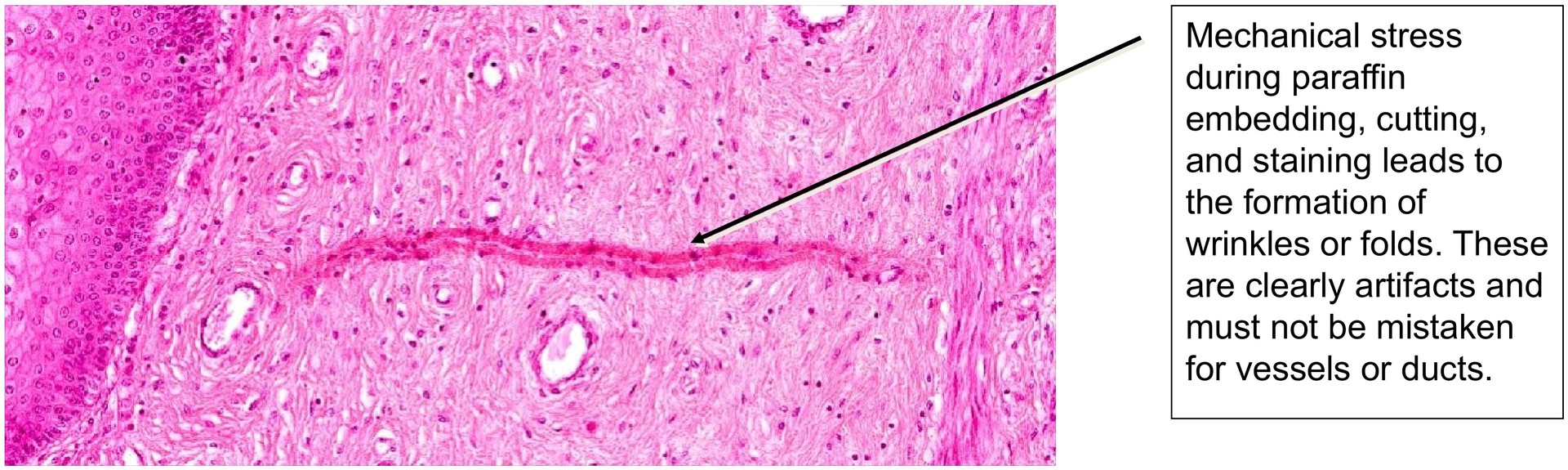
Review the two artefact images provided at the end of the document.
License
University of Basel
Downloads
