FEMALE REPRODUCTIVE ORGANS (ANATOMICAL MICROSCOPY)
10.3
Corpus luteum
Preparation:
Preparation Details:
Organ: Corpus luteum
Origin: Human
Staining: Van Gieson
Method and Specimen Description:
Routine histological section stained with Van Gieson, a connective tissue stain that colors collagen fibers red and muscle cells yellow. The cells of the corpus luteum also appear yellow.
Aim of the Examination:
To recognize the structure and organization of the corpus luteum, which develops primarily from granulosa cells and, to a lesser extent, from theca interna cells. Also, to understand the formation and regression of the corpus albicans as a later stage of corpus luteum degeneration.
Special Features of the Preparation:
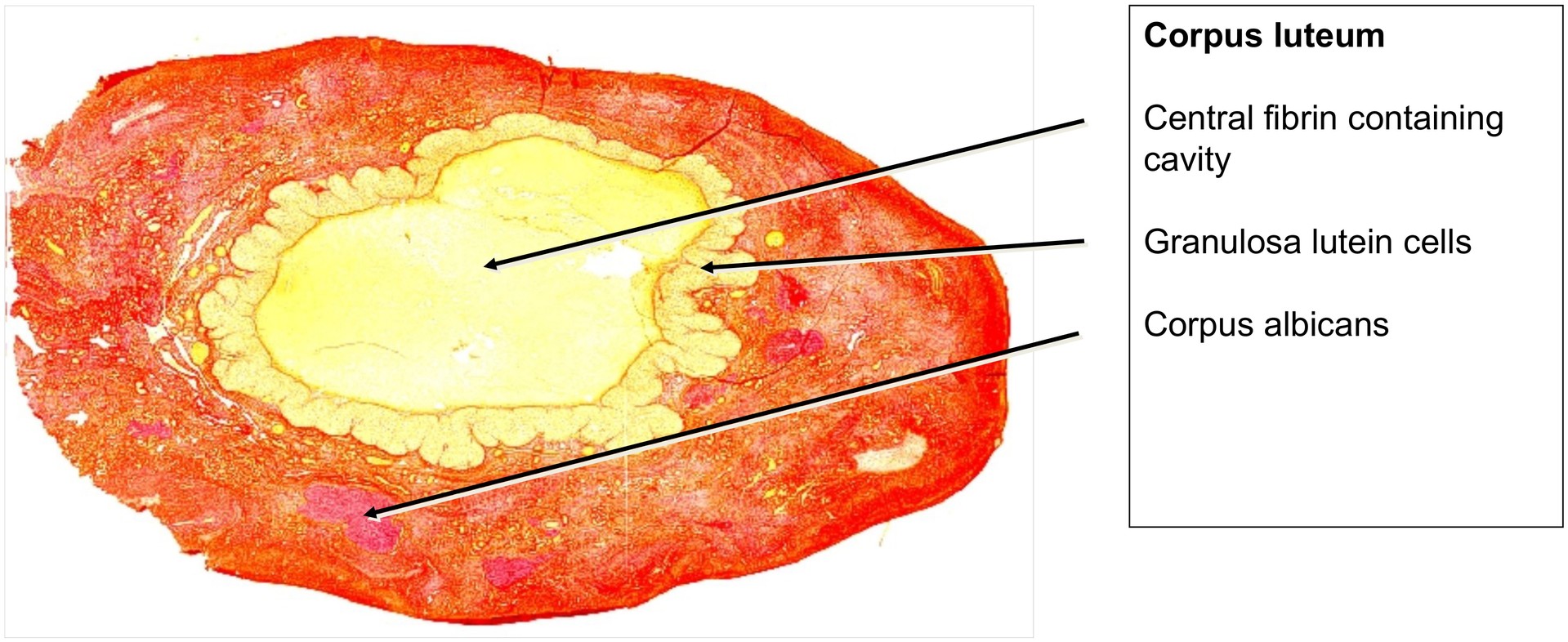
At low magnification, the corpus luteum is visible as the dominant structure within the ovary. At this stage of development, it is no longer recognizable as having originated from a Graafian follicle.
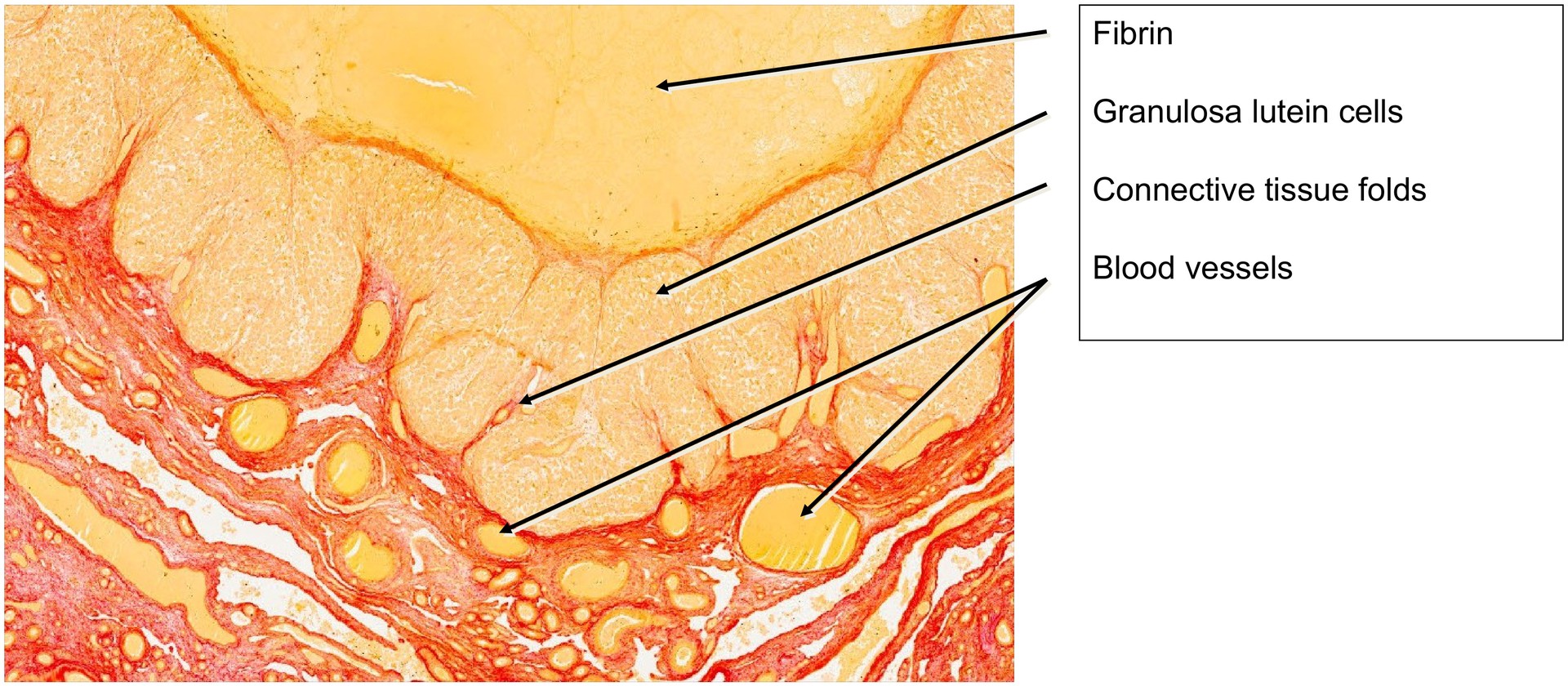
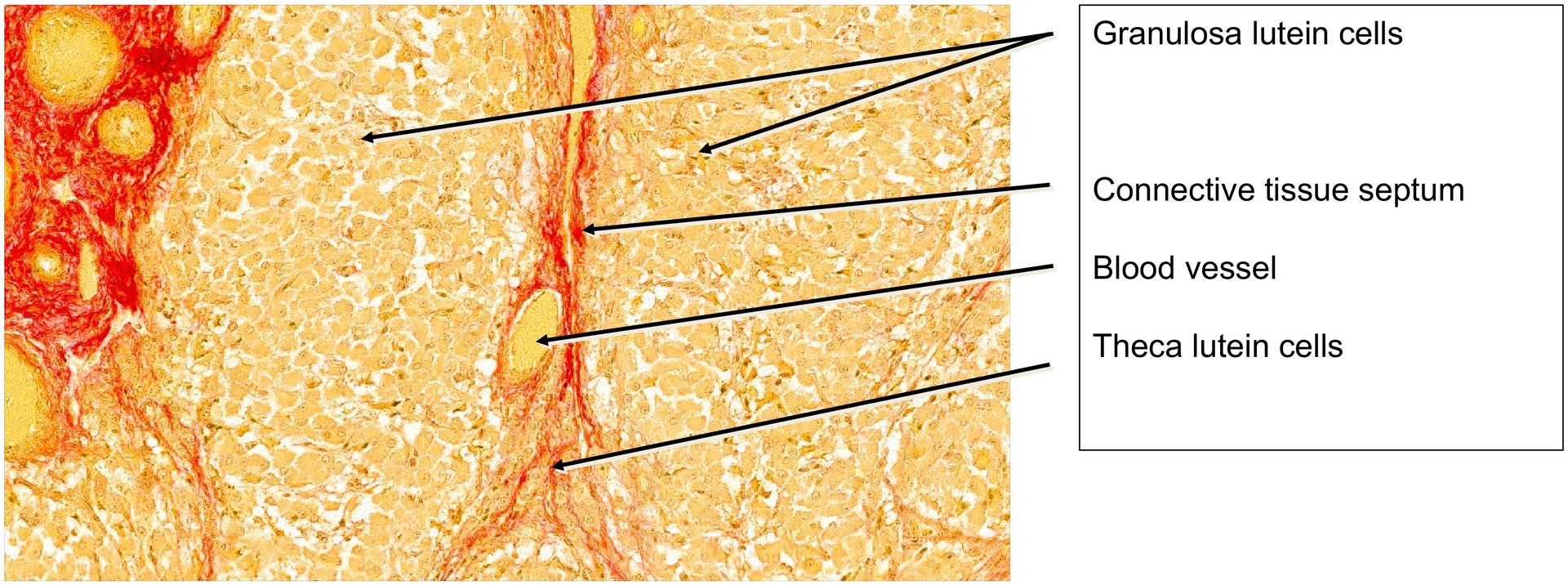
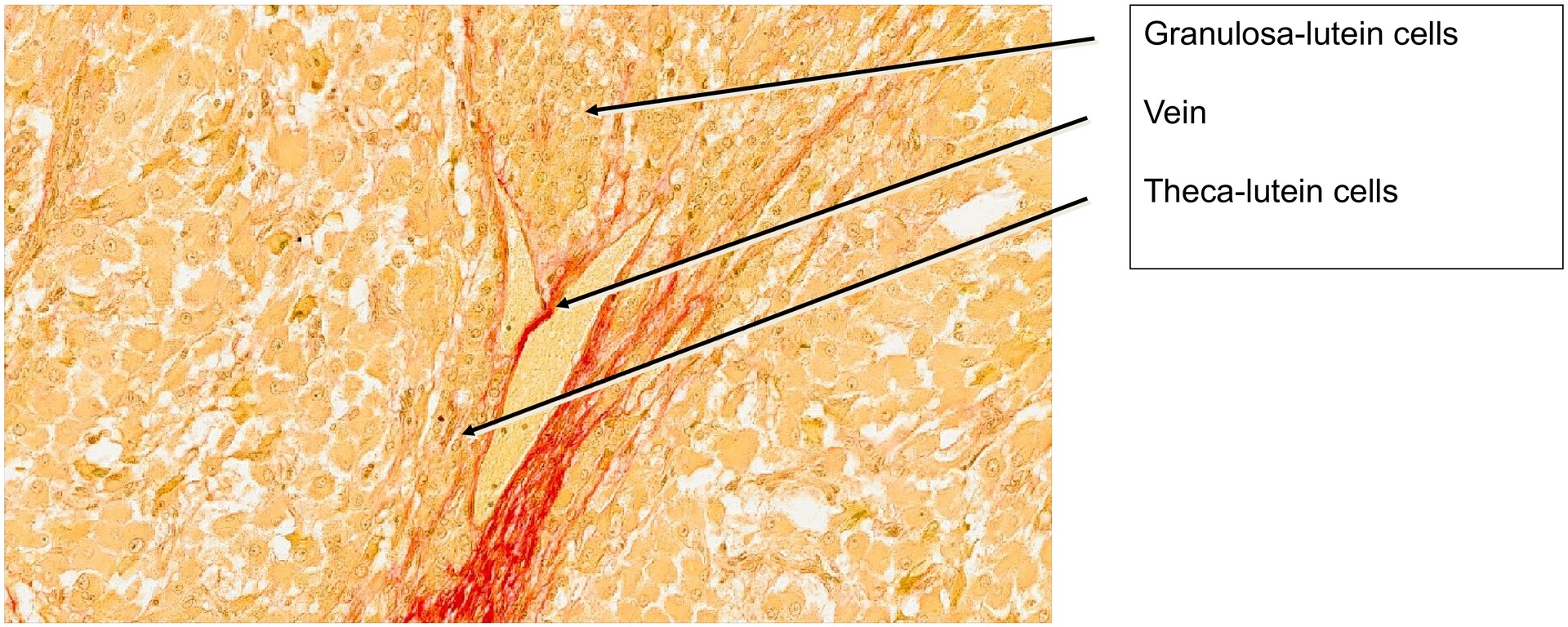
Under the influence of luteinizing hormone (LH), the granulosa cells of the follicle have enlarged and transformed into granulosa-lutein cells, which secrete progesterone, the principal corpus luteum hormone. The basal membrane of the Graafian follicle has largely dissolved, and the theca interna cells have differentiated into theca-lutein cells.
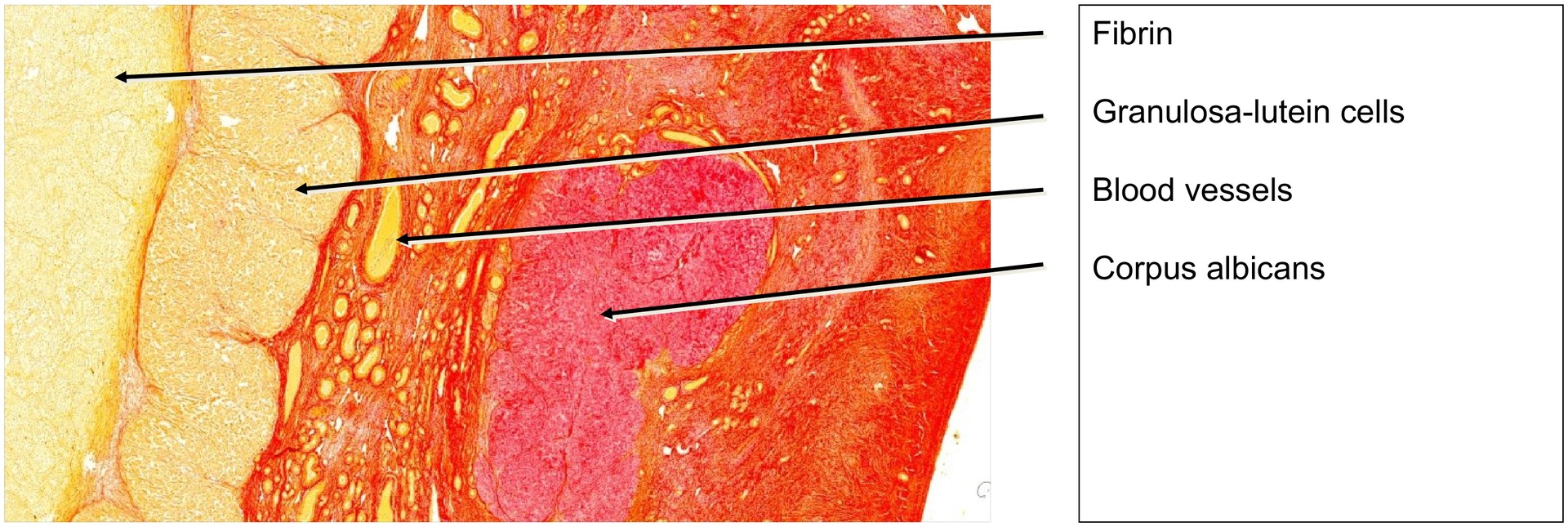
The rapid growth of the corpus luteum causes the wall to fold extensively. Connective tissue and blood vessels invade these folds, often carrying theca-lutein cells deeper into the tissue. Some theca-lutein cells remain at the periphery, external to the granulosa-lutein layer.
Immediately following ovulation, the central cavity of the corpus luteum contains residual follicular fluid mixed with blood from ruptured vessels; this transient structure is sometimes termed the corpus hemorrhagicum (also called corpus rubrum).
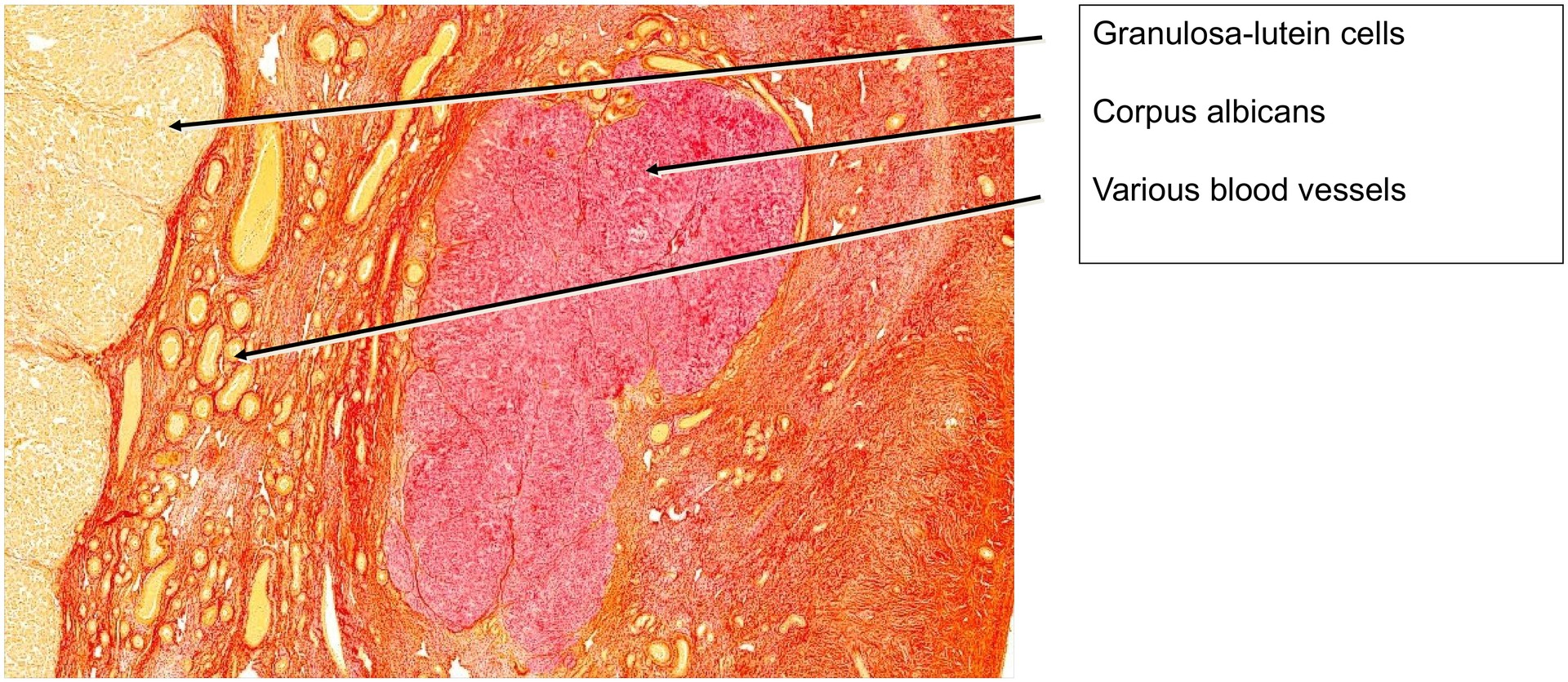
As development proceeds, fibrin is deposited within this cavity. During regression, the corpus luteum is gradually replaced by fibrous tissue, forming a corpus albicans. In this preparation, the central region consists mainly of fibrin. After approximately six weeks, the corpus luteum typically becomes a small, fibrous corpus albicans. With time, the corpus albicans itself degenerates, leaving only scar-like connective tissue.
Because regression occurs slowly, several corpora albicantia are usually visible within the same ovary—an observation also evident in this specimen.
Tasks:
• Examine the corpus luteum under low magnification and note its large size and folded structure.
• Identify the granulosa-lutein cells and locate theca-lutein cells at the periphery and within connective tissue folds.
• Trace the connective tissue strands between the folds and identify blood vessels within them.
• Observe the central region corresponding to the former follicular cavity and describe the appearance of the fibrin present.
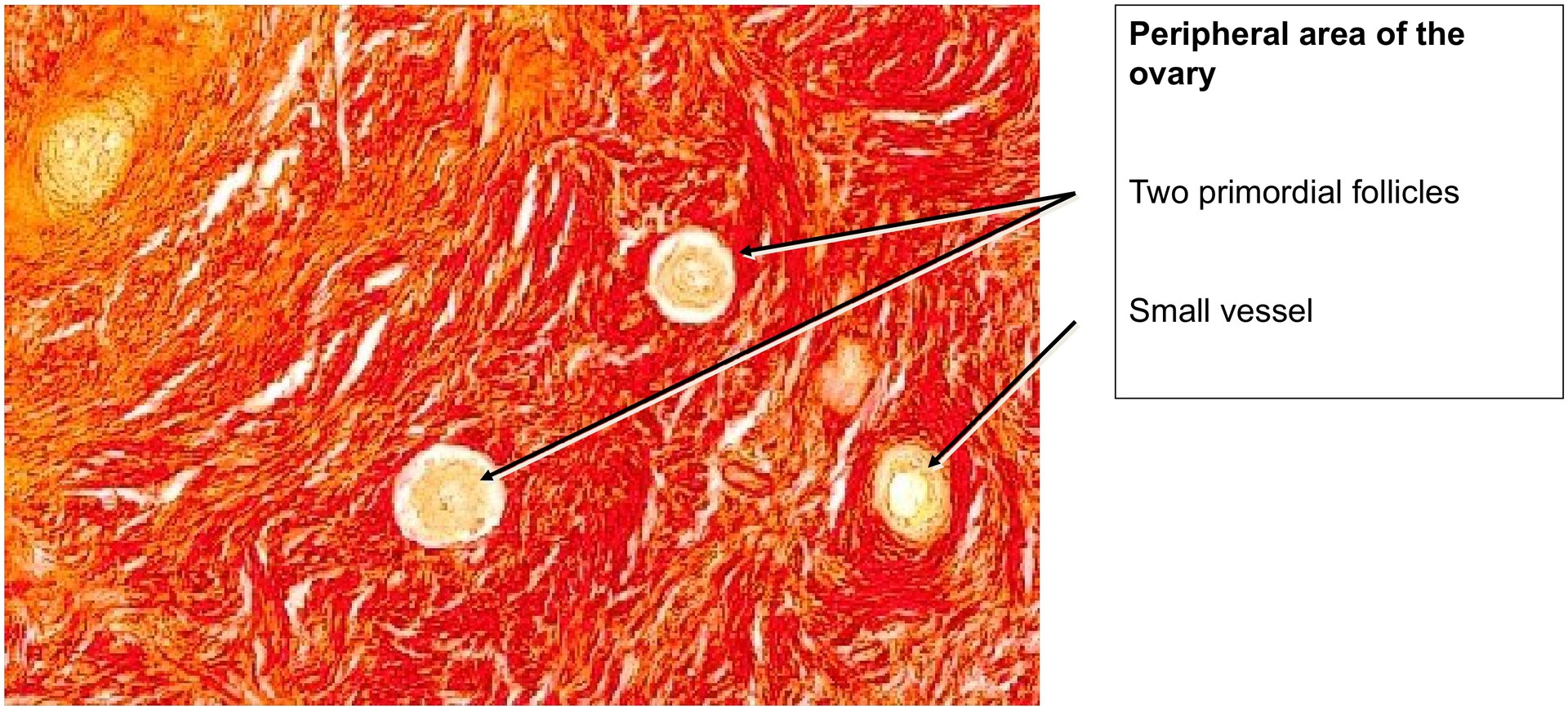
• Search the ovarian cortex for developing follicle stages (few may be visible).
• Identify one or more corpora albicantia and note their smaller, fibrous structure.
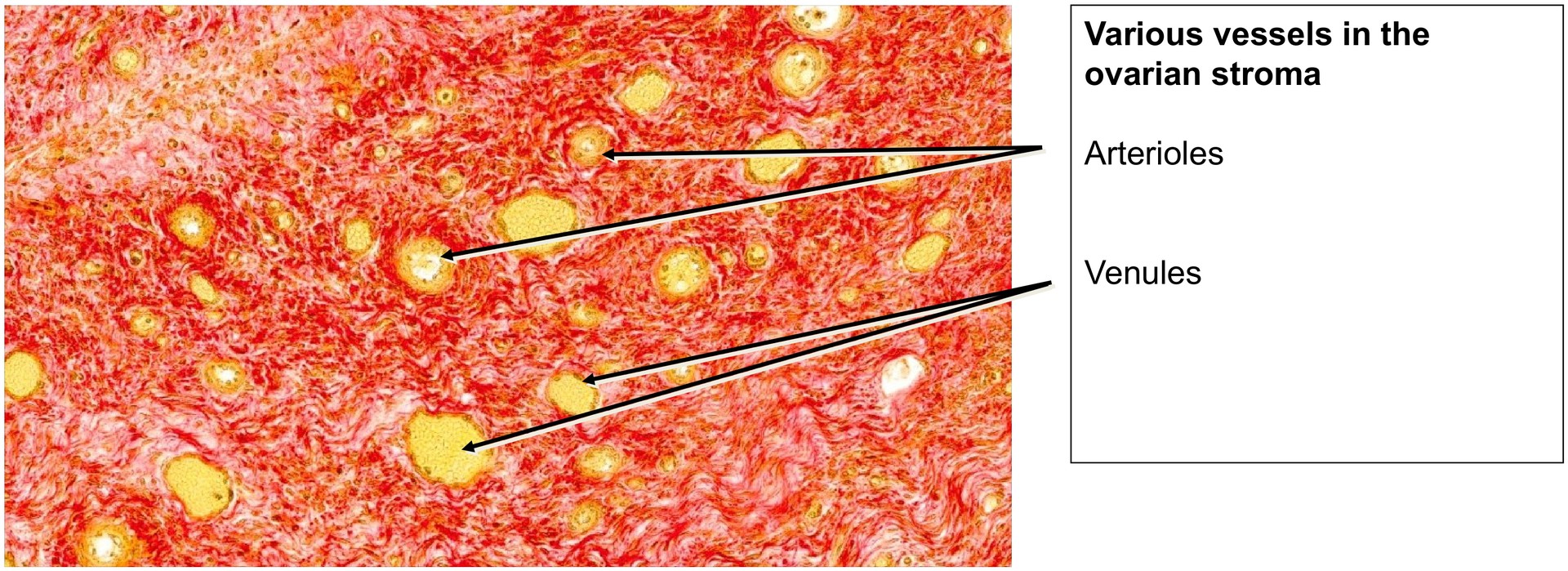
• Locate large and small blood vessels, which are present in considerable numbers throughout the corpus luteum.
License
University of Basel
Downloads
